Featured
Thyroid cancer, why does it occur and how to achieve 'cure
Thyroid Cancer: Why Does It Occur and How Do We Achieve 'Cure'? (Long Report)
Understanding Thyroid Cancer: 5 Key Q&A
Q1. What causes thyroid cancer?
The most clearly identified risk factor is a history of radiation exposure to the neck during childhood. Other factors like specific genetic disorders, family history, and iodine intake can also play a role, but in many cases, it's difficult to pinpoint a clear cause.
Q2. It's often called a 'good cancer'; is the prognosis really good?
Yes, for the most part. 'Papillary thyroid carcinoma' and 'follicular thyroid carcinoma', which account for over 95% of cases, have a very favorable prognosis, with a 5-year survival rate close to 99% even if the cancer has spread to nearby lymph nodes. However, there are rare types with poor prognosis, so accurate biopsy results are crucial.
Q3. Do I have to have surgery if diagnosed?
No, that's not the case anymore. Nowadays, if the cancer is very small (less than 1 cm) and is a low-risk papillary carcinoma, the global standard treatment has become 'active surveillance' rather than immediate surgery. Of course, depending on the size, location, and type of cancer, surgery may still be necessary.
Q4. Do all patients receive radioactive iodine treatment after surgery?
Not necessarily. Radioactive iodine treatment is selectively administered to patients who have had their entire thyroid removed and are at high risk of recurrence to lower the recurrence rate. If the risk of recurrence is low, it may not be necessary.
Q5. What exactly does 'cure' mean?
Medically, it is referred to as a 'remission state close to cure'. This means that after surgery or additional treatment, blood tests (thyroglobulin levels) and imaging tests (such as ultrasound) show no evidence of remaining cancer, and the risk of recurrence is very low. However, even then, regular follow-up is necessary for several years.
The Standard Journey of Thyroid Cancer: From Diagnosis to Treatment
Most journeys begin with the discovery of a small nodule (nodule) in the thyroid during a health check-up. Not all nodules are cancerous, but in suspicious cases, additional tests are conducted to determine if it's cancer and what type.
Step 1: Discovery and Classification
The most basic tests are neck ultrasound and 'fine needle aspiration (FNA)'. The ultrasound assesses the shape of the nodule, and a thin needle is used to collect a small sample of the nodule's cells for microscopic examination to check for cancer cells. If cancer is diagnosed, a treatment plan is established based on the type of cancer (papillary, follicular, etc.), size, and surrounding invasion.
Step 2: Treatment Dilemma - Surgery vs. Active Surveillance
Here comes a crucial moment of choice. In the past, it was common to undergo surgery if diagnosed with thyroid cancer, but that has changed.
- Active Surveillance: If the cancer is very small (less than 1 cm) and is a 'low-risk papillary carcinoma' with no evidence of spread, it's possible to monitor it with ultrasounds every 6 months to a year instead of immediate surgery. Decades of research data have shown that watching it this way rarely leads to metastasis or life-threatening situations.
- Surgery: If the cancer is large, poorly located, or has a high risk of recurrence, surgery is the standard treatment. If the cancer is only on one side, a 'lobectomy' is performed, while a 'total thyroidectomy' is done if it is on both sides or poses a high risk.
Episode: The Choice of Office Worker Lee Soo-jin in Her 30s
Lee Soo-jin, an office worker in her 30s, was diagnosed with a 7mm papillary thyroid carcinoma during a health check-up. The doctor explained two options: 'active surveillance' and 'lobectomy'. "At first, the idea of leaving the cancer in my body was very unsettling. However, after seeing the 10 and 20-year follow-up data the doctor showed me, I became confident that there would be no difference in prognosis if I delayed surgery." She chose active surveillance, and a year later, the cancer remains almost unchanged.
Step 3: Post-Surgery Management and the Journey Towards Cure
Does everything end after successful surgery? No, now begins the long-term management to prevent recurrence and maintain health. If the entire thyroid is removed, patients will need to take thyroid hormone medication for life, and radioactive iodine treatment may be added depending on the risk of recurrence. Regular blood tests and ultrasounds will then continue to check for any remaining cancer cells, ensuring the patient reaches a state of 'no evidence of disease (NED)'.
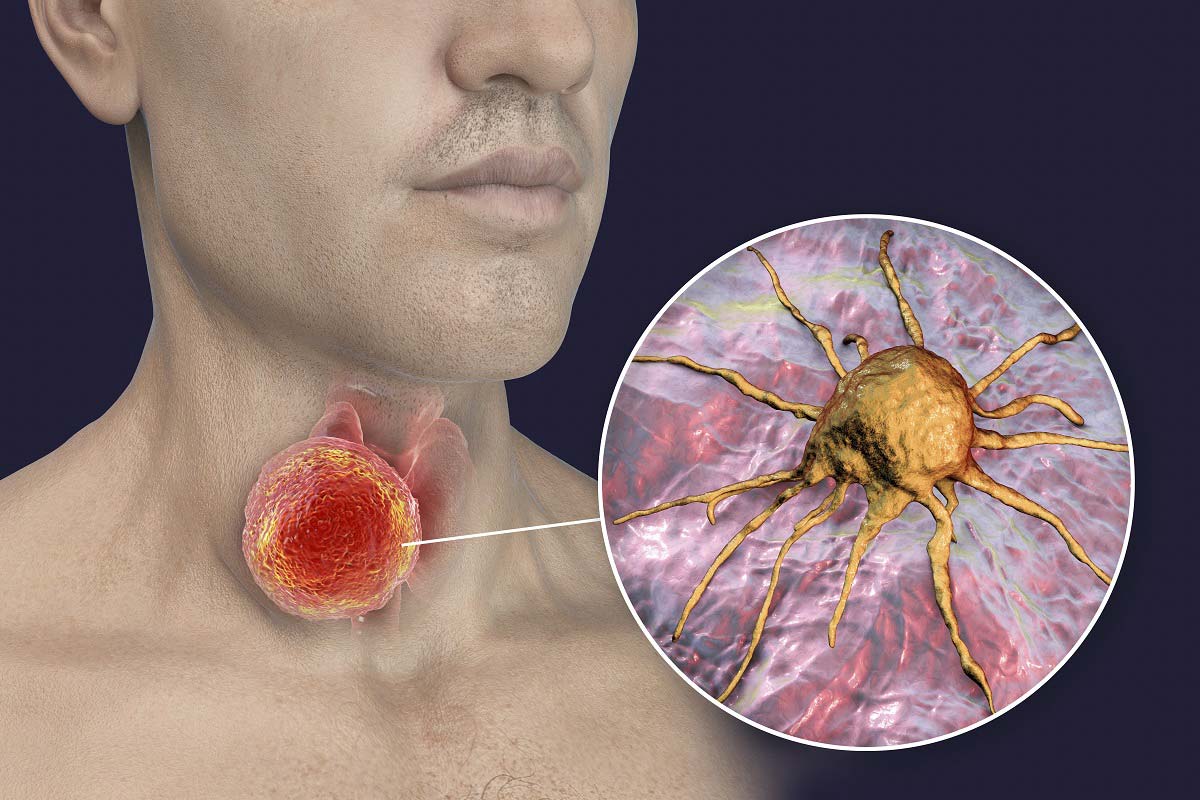
But why has the diagnosis rate increased so much? Let's take a look at the heated debate surrounding thyroid cancer.
In-Depth Exploration: Why Is Thyroid Cancer at the Center of the 'Overdiagnosis' Controversy?
Over the past 20 years, the incidence of thyroid cancer has exploded in several countries, including South Korea. However, the strange thing is that while the incidence skyrocketed, the mortality rate remained almost unchanged. Scientists and doctors attribute this phenomenon to 'overdiagnosis'.
Overdiagnosis refers to the premature and excessive detection of cancers that may never pose a threat to life and that individuals might have lived their entire lives without knowing. With the widespread use of health check-ups and significant advancements in ultrasound technology, even tiny 'micro-papillary cancers' that were previously undetectable have been discovered.
The problem is that most of these micro-papillary cancers grow very slowly or may not grow at all, often referred to as 'turtle cancers'. As unnecessary surgeries lead to lifelong dependence on thyroid hormone medications or complications such as damage to the vocal nerve, the fundamental question arises: "Is it always right to detect and treat all cancers early?" After much consideration, 'active surveillance' for small low-risk thyroid cancers has become the new standard instead of immediate surgery.
Episode: Reflections of Retired Doctor Kim Young-chul
Retired surgeon Kim Young-chul views the overdiagnosis debate with complex feelings. "When I was younger, I learned that finding even a small cancer meant surgery was the best option for the patient. But decades later, I've seen many patients live healthily without surgery. Medicine seems to be a long journey toward finding answers. Today's 'active surveillance' is a valuable lesson we learned from patients' lives in the past."
Common Misconceptions About Thyroid Cancer (FAQ)
Q. Is it serious if it has spread to the lymph nodes?
In the case of papillary thyroid carcinoma, lymph node metastasis is relatively common. While it is not a good sign, unlike other cancers, lymph node metastasis does not typically have a critical impact on survival rates. The risk of local recurrence may slightly increase, but overall prognosis remains very good.
Q. Can my voice change after surgery?
The vocal nerve runs just behind the thyroid. Therefore, if this nerve is affected during surgery, there may be temporary or permanent changes to the voice. However, if a skilled surgeon performs the operation, the risk of severe nerve damage is very low, around 1-2%. Choosing a hospital with extensive surgical experience is crucial.
Q. Will I never be able to eat seaweed soup again after thyroid cancer surgery?
No, this is a common misconception! Avoiding iodine-rich seaweeds is only necessary for a specific period before 'radioactive iodine treatment' after surgery. Once that treatment is completed, a balanced diet is generally recommended without the need for special restrictions on iodine intake.
Author Information: The content of this article is based on the official guidelines of the American Thyroid Association (ATA), the National Comprehensive Cancer Network (NCCN), and survival statistics from the National Cancer Institute (SEER), as well as long-term follow-up studies on active surveillance, providing an objective overview of the causes, treatment, and journey to cure thyroid cancer.
Recommended Reading
Popular Posts
The reason it took me a year to complete my first indie game
- Get link
- X
- Other Apps
Mabinogi Mobile - User Reactions and Global Release Schedule
- Get link
- X
- Other Apps

Comments
Post a Comment